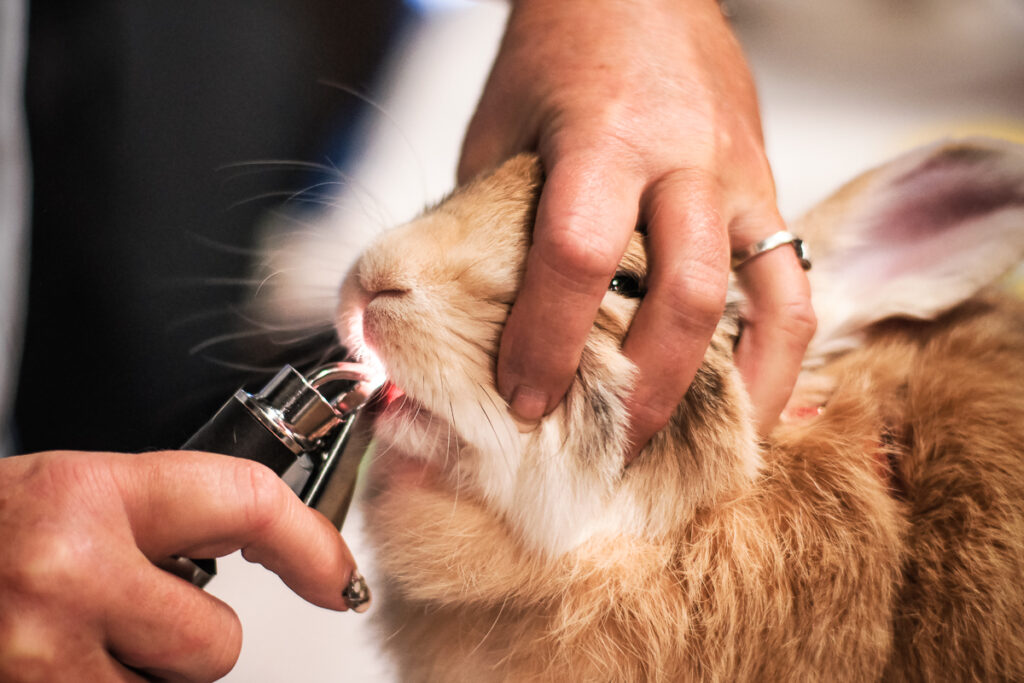
CC-remixed by Paige Parsons based on WabbitWiki’s CC Teeth article.
Dental problems are one of the most common medical issues in rabbits.1,2 The exact cause of dental disease in rabbits is unclear, although it is likely to be multifactorial and involve the following:3
- Inadequate teeth wear due to insufficient coarse fiber in the diet.
- Nutritional deficiency, including calcium, vitamin D, vitamin A, magnesium and protein.
- Genetic disposition—Netherland Dwarfs and lop-eared rabbits with flat faces seem to be especially susceptible.
An Oral Overview4
Rabbits have a total of 28 teeth: 4 incisors (those are the big choppers up front; what you picture when you think of ‘bunny teeth’). There are 2 of those on the top and 2 on the bottom. These are the teeth they use to chunk off mouthfuls of food…or to bite through phone cables!
Right behind the top incisor teeth are 2 small peg-like teeth called auxiliary incisors or ‘peg teeth’. They also help with severing things, especially if it’s something tough that needs more than just a quick snip.
They also have 6 upper and 4 lower premolars, then 6 molars up top and 6 more molars down below. Collectively, these 22 teeth further back in their cheeks are known as ‘cheek teeth’. Just as with our own premolars and molars, they’re used to grind food, readying it to be swallowed and digested.
Unlike us, however, rabbits have teeth that never stop growing, so it’s not just that they *like* to bite and chew – though they do – but it’s actually a necessity for them. They MUST continually wear down their teeth or, trust us, there will be much dental badness and huge vet bills!
You can help your bunny care for their teeth by feeding the roughest cut hay they’re willing to eat (1st cut takes the most biting and cutting work, 3rd cut is the softest and often suggested for old rabbits or ones who already have tooth trouble of one kind or another; 2nd cut is in between) and providing lots of tempting chew toys.
Properly maintained, all those teeth are SHARP! Every time we get a glimpse of them, we can’t help thinking, “Boy, it’s a really good thing they like us!”
Preventative Dental Care5
- Ensure growing rabbits have sufficient calcium and vitamin D. Growing rabbits are most susceptible to metabolic bone disease. Calcium should be 0.5-1.0% of the diet to provide sufficient calcium for the mineralization of growing teeth and surrounding bone.
- Provide unlimited fibrous foods such as grass and hay. Hay should be of a good quality. Calcium in poor-quality hay can be as low as 0.25% which is lower than the 0.44% dietary requirement for bone mineralization.
- Feed at least 3 types of fruits or vegetables a day, including one type of fibrous vegetables such as broccoli, cabbage, spring greens, spinach, or cauliflower leaves. Root vegetables and fruit, such as carrots and apples, are poor sources of calcium and should only be used as treats.
- Do not allow rabbits to select low-calcium cereals and legumes from muesli pellet mixtures. [Ed note – That’s the equivalent of junk food for rabbits.] Palatable extruded or pelleted diets are preferable as they prevent selective feeding. High calcium supplements should be avoided due to the risk of urine slugging.5
Online Support for Dental Issues
Facebook, Rabbit dental support group (Private group)
Video: Rabbit Dental Exam & Various Dental Problems
Dental Problems
Dental irritation
Sometimes rabbits may get food or objects stuck in their mouth or teeth, and it can cause alarming behavior with excessive lip-licking and head throwing as the rabbit tries to loosen and remove the stuck object. Rabbits should be taken to a rabbit-savvy veterinarian for a professional assessment if this behavior is persistent or re-occurring as it may be a sign of more serious dental issues.
Examples of this type of behavior:
- u/WickandFable. (2021). Behavior: (Medical) Dental Irritation – Excessive Lip-Licking
- u/DKMR. (2021). He throws his head back when eating some fruits like apples, the vet keeps telling me he’s ok during checkups… Any experience with this behaviour?
A Holland lop was found with their tongue hanging out in the morning, and a closer examination showed that a piece of spinach was stuck in their mouth.
Drooling
The medical term for drooling is ptyalism. Caregivers will often find perpetually wet spots around their rabbit’s mouth and on their chin. When left wet long enough, the area may eventually lose fur and develop moist dermatitis.
Lop and dwarf breeds may be prone to having a long-lasting wet chin when drinking from a bowl or eating wet vegetables and not grooming themselves properly afterwards. Caregivers can help by manually wiping their chins with a towel and consider switching them to water bottles to prevent the issue from reoccurring.
Dental issue drooling should also not be confused with an over-reactive scent gland under the rabbit’s chin. Some rabbits may be overenthusiastic with their claiming of territory and rub their chin to irritation.
See the links below for more information about drooling in rabbits.
- MediRabbit, Differential Diagnosis for Ptyalism
- MediRabbit, Esther van Praag, Ph.D., Excessive secretion of saliva and coughing
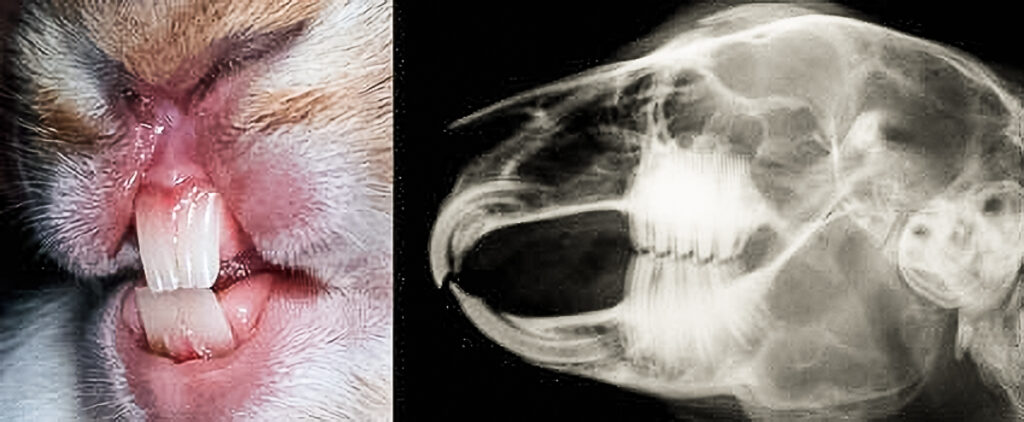
Malocclusion
Malocclusion occurs when a rabbit’s teeth do not meet each other properly. Typical treatment for this condition are regular teeth trims or removal of problematic teeth. See the main article for more details.
While encouraging teeth wear with chewing hay and other fibrous materials may help slow down the rate of overgrown incisors and molar spurs from developing, some rabbits are born with (or develop from physical trauma) severely misaligned teeth such that the issue will continuously reoccur throughout their lifetime and require ongoing medical procedures to keep the rabbit comfortably eating on their own.
Never attempt to trim your rabbit’s incisors at home. This can seriously harm your rabbit and cause pain and irreversible damage.
Frequently observed dental problems from self-trimming with a cutter or nail clipper include the following:7
- Sharp edges, that can hurt the rabbit when eating or grooming.
- Stress fracture or longitudinal cracks in the tooth, either in the visible part or under the gum line.
- Tooth growth stopping due to damage of the tooth root (endodontic diseases).
- Exposure of the dental pulp resulting in pulpitis (inflammation of the most internal part of a tooth, the dental pulp).
- Abscessation and changes of the surrounding tissues and the alveolar bone.
- Fracture of the jaw bone.
- Pain due to the sudden concussion of the dental pulp and nerves in the periodontal and periapical tissues surrounding the tooth root, due to the enormous amount of energy released into the tooth during the clipping.
The following are more articles about why not to trim incisors at home without professional medical tools:
- MediRabbit.com. Never trim the incisors of your rabbit yourself !!!
- Bunny Brigade Inc. (2023). Surgical footage of a rabbit that had to undergo 5 surgical procedures after owners attempted to trim teeth on their own. (Graphic)
Video: Do Rabbit Teeth Need to Be Trimmed?
Extra resources
Incisor removal
For rabbits that require regular incisor trims, removing the problematic incisors completely may be a good choice as a semi-permanent solution, although the upfront cost may be high. The surgery should be completed by a rabbit-savvy veterinarian experienced in the procedure to reduce the risk of missing teeth remnants in the gums – any teeth parts left can regrow into full teeth again and require trims and another extraction again.
Overgrown teeth roots
In other cases, overgrown teeth roots can be the cause of many health issues such as weepy eyes, sneezing, and anorexia. When severe, teeth roots can grow into the eyes and cheeks and even break the skin. This condition cannot usually be diagnosed with a visual check by a veterinarian and requires more advanced imaging such as radiographs and CT scans.
Overgrown teeth roots should be treated with pain management and, ultimately, surgical removal if appropriate.
The following are some resources about rabbits with overgrown teeth roots:
- IMV Imaging. (2022). Case Study – The Inappetent Rabbit
- Long Beach Animal Hospital. (2019). Rabbit Teeth Conditions (Graphic)
Dental abscesses
(For a full discussion of dental Abcesses, Learn more from WabbitWiki.)
Many kinds of trauma and dental issues like malocclusion can develop into dental abscesses.
- Dr. Honzelka. Dental (tooth) Abscesses in Rabbits
- R. Avery Bennett, DVM, MS, DACVS. (2009). Managing dental abscesses in rabbits (Proceedings)
- PetMD. (2008). Apical Abscesses in Rabbits
Further reading
- Jennifer Hamlin. (2013). Causes, examination and treatment of dental disease in rabbits
- Bishops Stortford Veterinary Hospital. How to check your rabbit’s teeth
- Robin Rysavy, DMA in consultation with Brock Exline, DVM. (2016). Rabbit Teeth: How They Work
- Dale Kressin, DVM, FAVD, Dipl. AVDC. Anatomy of rabbit teeth
- MediRabbit. Healthy rabbit dentition
- A. Meredith. Rabbit Dentistry [PDF]
- Frank J. M. Verstraete, DrMedVet & Anna Osofsky, DVM. (2005). Dentistry in Pet Rabbits [PDF]
- Animal Dentistry & Oral Surgery Specialists LLC. Rabbits & Rodent Dental Care
- Charky and Ash. Pictures of Rabbit Teeth
References
- PetMD. Common Medical Diseases in Rabbits. ↩︎
- VetWest Austrailia. Common Medical Disease in Rabbits. ↩︎
- Keeble, E & Meredith, A. (2006). Rabbit medicine & surgery: Self-assessment color review. ↩︎
- Posted on FB by Bunanza Rabbit Rescue Ranch and Adoption Center on September 13th, 2020 ↩︎
- Varga, M. (2013). Textbook of rabbit medicine. (2nd ed.). ↩︎
- Varga, M. (2013). Textbook of rabbit medicine. (2nd ed.). ↩︎
- MediRabbit.com. (n.d.). Never trim the incisors of your rabbit yourself !!! Retrieved 29 Apr 2020 from http://www.medirabbit.com/EN/Dental_diseases/Treatment/Clipping.htm ↩︎
All About Teeth: Preventative Care & Dental Problems in Rabbits by Paige K Parsons, Rabbit.org Foundation, WabbitWiki is licensed under CC BY-SA 4.0